Bladder Cancer in dogs: The urinary system consists of the kidneys, bladder, urethra, and bladder. The kidneys are the organs that filter blood to remove waste and maintain the body’s electrolyte balance.
Table of Contents
The filtered waste turns into urine, travels through the ureters to the bladder, and collects continuously in the bladder.
The bladder can expand due to the special properties of its wall and inner membrane. When an animal urinates, urine is emptied from the body through the bladder.
What is bladder cancer in dogs?
The most common variant of bladder cancer is transitional cell carcinoma (TCC). It is a tumor of cells located inside the bladder.
Other less common tumors of the bladder may include leiomyosarcomas, fibrosarcomas, and other soft tissue tumors.
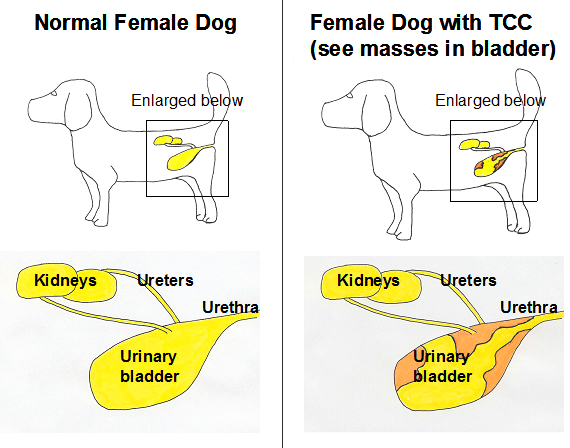
TCC can also be found in the kidneys, ureters, urethra, prostate, or vagina. It spreads to the lungs, lymph nodes, bones, or other organs (metastasis).
Approximately 20% of dogs with bladder cancer have metastases at diagnosis. Bladder cancer is more common in dogs than in cats, but less than 1% of cancers are reported in TCC dogs.
Also Read: Dog Breathing Fast? Tachypnea in Dogs! Treatment
Some studies have suggested that long-term exposure to certain chemicals (petrochemicals, pesticides) may increase a dog’s risk of developing bladder cancer.
Clinical signs
The signs of bladder cancer are similar to those seen with urinary tract infections. These include short, frequent urination, painful urination, bloody urine, and incontinence.
Symptoms often improve with the administration of antibiotics (since bladder infection is a common joint disease) but recur after a while.
A veterinarian may experience a tumor when the abdomen touches if the abdomen is large. If the tumor has spread to the lymph nodes inside the abdomen, it can be touched on a digital stool test. The tumor may spread to the bones or cause bone pain.
If a bladder tumor enters the bladder, it obstructs the flow of urine and causes urination. If severe enough, it can eventually lead to kidney damage (hydronephrosis) and kidney failure.
Complete inability to urinate is a medical emergency and should be resolved immediately by a veterinarian.
Diagnosis for bladder cancer in dogs
Urination
Pets with bladder cancer sometimes have cancer cells in their urine. Inflammation of the urinary tract from infection forms cells that look similar, so this test is rarely a diagnosis for bladder cancer.
However, urination can check for secondary infections of the bladder (due to tumors) and help assess kidney health.
Blood work
Blood work is often normal in pets with bladder cancer if kidney function is not impaired. But blood work is important because it can help assess the overall health of your pet, which can have an impact on treatment options.
Veterinary Bladder Tumor Antigen (VBTA) Test
This is a urine test to check for bladder cancer in dogs. One of the risks of this test is that dogs that do not have bladder cancer can be tested positive for VBTA, especially if they have a bladder infection.
Abdominal imaging
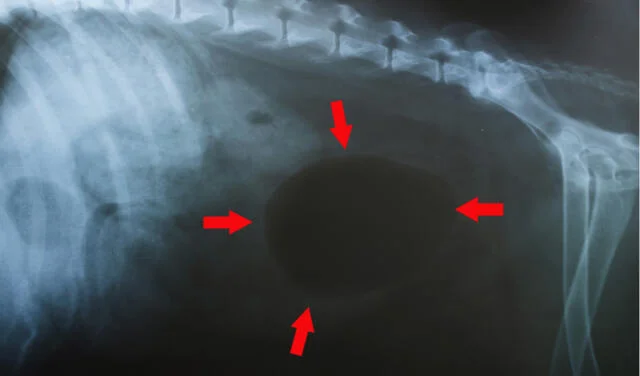
Bladder tumors are rarely seen on normal abdominal radiographs (x-rays), but tumor spread to the bones is obvious.
Special color studies (cystograms) can sometimes be used to make tumors visible on radiographs. This study can be very helpful if your veterinarian suspects that the tumor may be invading your pet’s bladder.
Ultrasound is another way to paint the abdomen. Ultrasound helps to see the size of the tumor in the bladder and the size of the lymph nodes adjacent to the bladder.
Chest Imaging
As bladder cancer spreads to the lungs, your veterinarian may take chest radiographs (x-rays) to check for metastases.
Biopsy
To accurately diagnose TCC of the bladder, a sample of cancer cells should be evaluated.
This is usually done with a surgical biopsy or from cells collected through an ultrasound-guided urinary catheter.
In female dogs, cystoscopy (a camera inserted into the bladder) can be used to see the tumor live and make a biopsy.
The biopsy is sent to the pathologist for examination under a microscope.
Treatment for bladder cancer in dogs
Surgery: Surgical removal of the entire tumor is very rare. The tumor usually arises at the site of entry into the bladder and the lower truffle area of the bladder.
As a result, surgery interferes with these vital structures. Occasionally the tumor arises elsewhere in the bladder (especially in cats), and the surgery can dispose the tumor completely.
This is called “debulking” when the tumor is reduced only in size during surgery. Although this may temporarily relieve the pet’s symptoms, the tumor may grow back.
Chemotherapy: Unfortunately, the chemotherapy protocol that works best for bladder cancers in pets has not yet been found.
Less than 20% of pets respond to the intravenous chemotherapy protocols currently in use.
Some oral nonsteroidal anti-inflammatory drugs, such as Piroxicam (Feldene) or Meloxicam (Metacom), have demonstrated anti-cancer activity with TCC and may help some dogs.
These work best when combined with chemotherapy.
Radiation Therapy: Radiation therapy can help some patients with bladder cancer. Although some studies suggest that it works better than chemotherapy, it can cause serious side effects.
Causes of bladder cancer in dogs
The exact cause of bladder cancer in dogs is not known, but there seems to be a link between genetic predisposition and long-term exposure to herbicides such as pesticides and herbicides.
Symptoms of bladder cancer in dogs
Bladder cancer in dogs can be a bit tricky to diagnose because the common symptoms of the disease mimic other urinary tract conditions such as stones or infections.
If your puppy has developed bladder cancer you may notice one or more of the following symptoms:
- Urinating small amounts
- Difficulty in urinating
- Accidents at home
- Colorless or bloody urine, or
- Chronic urinary tract infections resistant to treatment
In the later stages of bladder cancer, some dogs become lethargic to cancer that has spread to the bones or lungs.
Prognosis
Chronic prognosis is usually low in pets with bladder cancer regardless of treatment. However, with treatment, pets can improve their quality of life for a while.
On average, dogs with TCC of the bladder live 4-6 months without treatment, and 6-12 months with treatment.
FAQs on Bladder Cancer in Dogs
What causes bladder cancer in dogs?
Bladder cancer in dogs can be caused by a variety of factors, including genetics, exposure to certain toxins, or infections. In some cases, the underlying cause may be unknown.
What is the prognosis for bladder cancer in dogs?
The prognosis for bladder cancer in dogs can vary widely depending on the type and stage of cancer, as well as the overall health of the dog. In general, the earlier the diagnosis and treatment, the better the prognosis.
What are the symptoms of bladder cancer in dogs?
Symptoms may include blood in the urine, difficulty urinating, frequent urination, and pain while urinating.
For more information on this topic, please talk to your veterinarian who treats your pet.
References
https://academic.oup.com/ilarjournal/article/55/1/100/847848?login=true
https://academic.oup.com/aje/article-abstract/104/6/673/139416

